Artificial Intelligence in Healthcare: Market Overview and Strategic Insights
Market size & growth projections
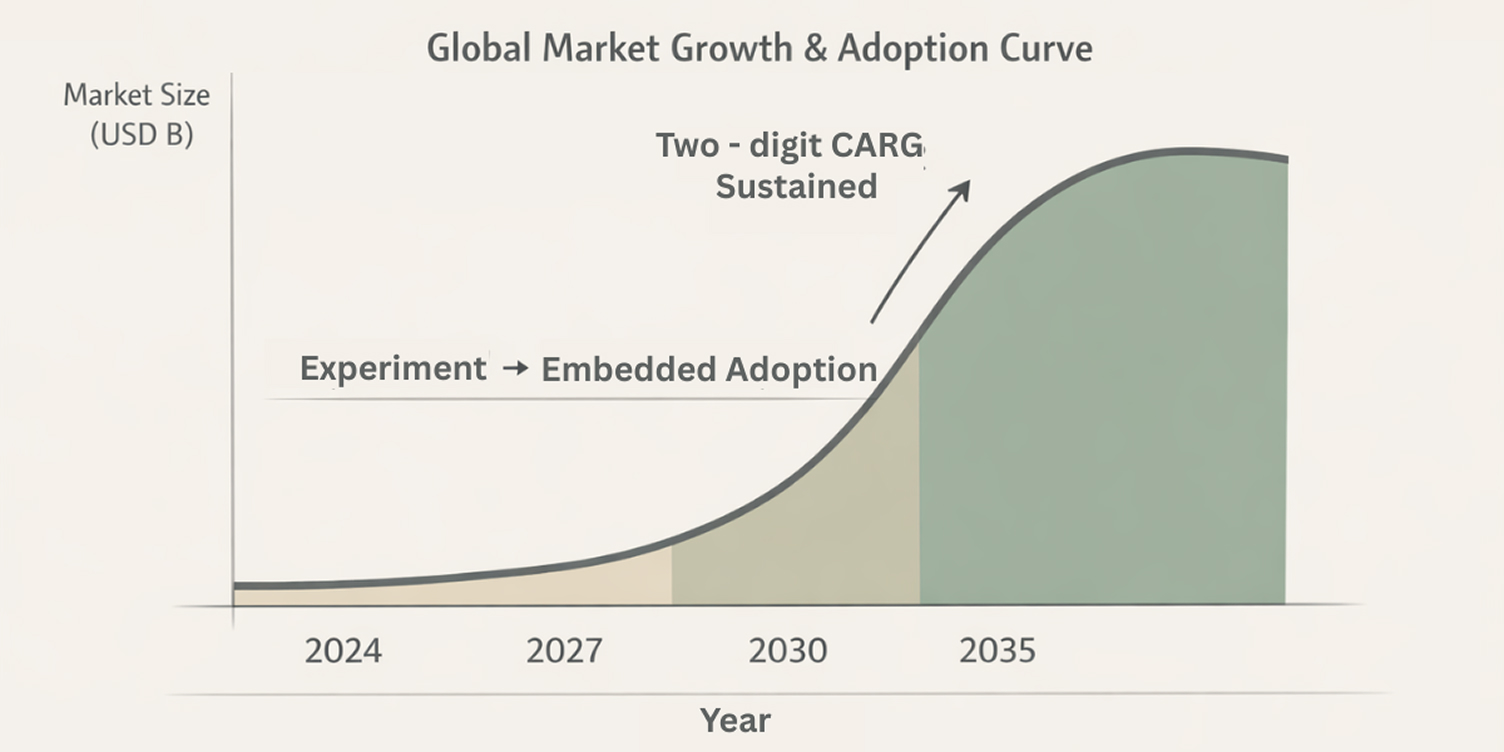
The artificial intelligence in healthcare market has moved beyond experimental adoption into measurable economic expansion worldwide.
Multiple independent forecasts show the market’s value increasing sharply over the next decade:
One comprehensive estimate projects the global market at USD 36.96 B in 2025 and growing to USD 51.20 B by 2026, continuing toward USD 613.81 B by 2034 at about 37 % annual growth.
Another leading industry research group forecasts the market’s valuation at USD 21.66 B in 2025 with a trajectory to USD 110.61 B by 2030 at a compound growth rate exceeding 38 %.
Alternate analysis indicate smaller base figures but consistent growth trends, such as projections from USD 23.83 B in 2024 to nearly USD 79.13 B by 2030.
Regardless of baseline variation, independent sources consistently project two-digit annual growth through 2030 and beyond, signaling strong adoption across healthcare domains.
Diagnostics as an economic lever
.jpg)
Diagnostic accuracy and speed have become economic variables for healthcare systems.
Imaging volumes continue to grow faster than the specialist workforce, particularly in radiology, pathology, and cardiology.
According to Precedence Research, diagnostic imaging represents the largest application segment within the AI healthcare market, reflecting the urgency of this imbalance rather than preference for a specific technology.
What distinguishes recent adoption cycles is not that AI can interpret images, but that it measurably alters throughput and error rates.
Independent analyses show AI-assisted diagnostics improving detection accuracy by 15–20% in radiology workflows while reducing turnaround times by up to 50% in high-volume departments.
These gains directly affect hospital capacity utilization and downstream treatment costs.
This is why imaging AI has transitioned from optional add-ons to embedded workflow components.
Vendors are increasingly evaluated on integration depth rather than algorithm performance alone, a shift that favors long-term platform contracts over point solutions.
Why cancer care attracts disproportionate AI investment?
Cancer care illustrates how AI adoption concentrates where pressure is most acute.
Global cancer incidence is expected to rise steadily over the next two decades, increasing demand for earlier detection and more precise treatment planning.
AI systems addressing oncology workflows do so at multiple points: screening, pathology interpretation, treatment selection, and follow-up monitoring.
Statistical evidence supports this focus. AI-enabled cancer detection tools have demonstrated early-stage detection improvements of over 30%, while pathology automation reduces slide review time by more than 60%, accelerating clinical decision cycles.
In mammography alone, AI assistance has reduced false positives by roughly 25%, limiting unnecessary biopsies and follow-up procedures.
These outcomes explain why pharmaceutical and life sciences companies continue to acquire or partner with oncology-focused AI firms.
Reuters reported that AstraZeneca’s acquisition of an AI company focused on oncology research was driven by the need to accelerate biomarker discovery and clinical development timelines.
Why oncology AI scales faster?
Drug discovery
Drug development economics explain the sustained interest in AI across pharmaceutical research. Traditional discovery pipelines are costly, slow, and prone to late-stage failure.
AI’s value lies in reducing uncertainty earlier in the process.
Reuters reports that pharmaceutical companies are expanding AI usage in target identification, molecule screening, and trial design, aiming to reduce early-stage attrition and improve patient selection.
Studies indicate that AI-driven discovery platforms can cut initial screening timelines by nearly half while improving hit-to-lead ratios.
Regulatory agencies have responded by issuing clearer guidance on acceptable AI practices in drug development, reducing compliance uncertainty.
The result is a shift from experimental pilots to long-term AI platform partnerships across R&D pipelines.
Administrative AI
Clinical breakthroughs often dominate headlines, but administrative automation may represent the most stable source of AI demand.
In many healthcare systems, administrative expenses consume nearly one-third of total spending. AI deployment in this area targets documentation, coding, scheduling, and claims processing.
ResearchAndMarkets identifies administrative automation as one of the fastest-growing AI application areas, driven by staffing shortages and reimbursement complexity.
Hospitals using AI-assisted documentation report reductions of 30–40% in clinician documentation time, directly addressing burnout and throughput constraints.
Unlike clinical AI, these systems face fewer regulatory hurdles, accelerating adoption.
Administrative AI impact
This segment is underrepresented in competitor content despite its outsized influence on purchasing decisions.
Population health and public systems
.jpg)
At the population level, AI adoption reflects a different set of incentives. Governments and public health agencies are applying AI to disease surveillance, capacity planning, and long-term risk modeling.
Research highlighted by the Financial Times shows that AI models trained on longitudinal health records, which estimate susceptibility across hundreds of diseases decades in advance, outperform traditional risk tools in several categories.
These capabilities support the design of preventive policies rather than individual treatment decisions, positioning AI as a planning tool rather than a clinical assistant.
Market impact here is slower but more durable, supported by public funding cycles.
AI in the US healthcare market
Rising chronic disease incidence, persistent clinician shortages, reimbursement pressure, and administrative overload are forcing healthcare organizations to adopt systems that compress time, reduce error, and improve decision quality at scale.
This is why the US continues to lead global AI healthcare spending.
According to Precedence Research, North America accounts for the largest share of the global AI in healthcare market, driven primarily by hospital networks, pharmaceutical companies, and payer-provider organizations investing in automation and predictive systems.
Market trajectory
Asia-Pacific beyond India
Across Asia-Pacific, AI healthcare adoption is expanding rapidly due to aging populations and rising chronic disease prevalence.
Countries such as China, Japan, and South Korea are investing heavily in AI-assisted imaging, hospital automation, and drug discovery, supported by national AI strategies.
Market research consistently identifies Asia-Pacific as the fastest-growing regional segment, even though its absolute market size remains below North America.
Adoption favors high-throughput clinical AI, particularly in imaging and diagnostics, where AI mitigates clinician shortages and improves service reach.
India
AI adoption driven by scale and cost pressure India’s AI in healthcare market is developing under a different economic logic than the US.
While per-capita healthcare spending is lower, patient volumes, clinician shortages, and uneven access create strong incentives for automation and decision support. Industry research indicates India’s AI healthcare market is growing at over 40% CAGR, outpacing most developed markets.
Growth is concentrated in diagnostics, radiology outsourcing, population health analytics, and hospital operations, where AI offsets workforce gaps rather than augments existing capacity.
Government-backed digital health initiatives, including large-scale electronic health record programs and national health data platforms, have accelerated AI readiness.
As a result, AI deployment in India often appears first in screening, triage, and administrative automation, rather than advanced precision medicine.
This positions India as a high-growth implementation market rather than an early innovation hub.
Europe
European AI healthcare adoption reflects regulatory alignment and public system incentives rather than speed of commercialization.
Market analyses show Europe holding the second-largest share of global AI healthcare spending, with strong uptake in radiology, oncology decision support, and population health modeling.
Unlike the US, where hospital networks drive purchasing, European AI adoption is shaped by national health systems, which prioritize AI systems that demonstrate cost containment, fairness, and explainability.
As a result, AI platforms with transparent decision logic and validated outcomes see faster scaling across regions such as Germany, the UK, and the Nordics.
Growth remains steady rather than explosive, but once approved, AI systems tend to achieve longer contract durations and wider institutional penetration, reinforcing durable market demand.
Technology stack shaping AI adoption in healthcare
AI deployment in healthcare today relies on a layered technology stack rather than isolated models.
At the core are machine learning and deep learning systems, which support predictive analytics, image recognition, and risk scoring across clinical and administrative workflows
Core AI technologies in production use
NLP
- Computer vision underpins radiology, pathology, and dermatology applications, while natural language processing (NLP) enables clinical documentation, coding automation, and extraction of insights from unstructured medical records.
- These technologies dominate production use because they integrate directly into existing workflows and data formats.
- Research shows imaging and NLP-based systems account for the majority of deployed AI solutions, reflecting their immediate operational impact rather than experimental novelty.
Cloud, data infrastructure
- Cloud computing has become foundational to AI scalability in healthcare. Most enterprise deployments rely on HIPAA- and GDPR-compliant cloud environments to support model training, inference, and integration with hospital systems.
- Interoperability layers connecting AI tools to EHR systems, PACS, and claims platforms increasingly determine commercial success.
- Vendors that fail to integrate cleanly face resistance regardless of algorithm quality
- This has shifted competitive advantage from model performance alone to infrastructure compatibility and data governance maturity.
Life sciences technology stacks
- In pharmaceutical R&D, AI stacks combine deep learning, molecular simulation, and high-performance computing to accelerate target identification and compound screening.
- Studies indicate AI-driven discovery platforms can reduce early-stage screening timelines by up to 50%, while improving hit-to-lead conversion rates.
- This directly addresses one of the most expensive failure points in drug development.
- As a result, pharmaceutical companies increasingly enter multi-year platform partnerships rather than pilot projects, embedding AI systems into core discovery pipelines rather than treating them as experimental tools.
Implications for AI vendors
.jpg)
Measurable downstream impact is becoming a more important factor in determining vendor difference as healthcare customers advance in their implementation of AI.
Evidence from real-world deployments shows that vendors capable of embedding AI into operational decision loops, rather than delivering standalone predictions, are more likely to achieve sustained adoption.
For example, machine learning models trained on electronic health record data have been shown to reliably predict unplanned hospital readmissions with explainable performance metrics, enabling providers to identify high-risk patients early and support discharge planning and preventive care interventions.
In this case, the vendor's ability to incorporate risk scores into care coordination workflows which resulted in better outcomes and lower avoidable costs was more valuable than prediction alone.
Evidence from deployments shows that vendors prioritizing actionability over accuracy alone are better positioned to justify economic value to buyers.
Workflow-embedded AI outperforms assistive-only tools
Clinical AI providers that function as advisory overlays are consistently outperformed by those that integrate directly into current workflows.
According to The Lancet Oncology, AI-supported mammography screening reduced radiologists' effort by 44% while allowing them to identify 20% more breast cancers than with traditional double-reading.
The fact that AI outputs were incorporated straight into the reading process rather than being offered as independent analytical reports was the deciding factor.
This finding has important implications for vendors: AI systems that reduce cognitive load and decision latency are more likely to be retained long-term than tools that require clinicians to context-switch or reinterpret outputs.
Vendors increasingly evaluated on operational ownership
Evidence from scaled deployments indicates that healthcare organizations expect vendors to assume partial responsibility for system performance post-deployment.
Vendors that provide monitoring, model recalibration, and performance auditing reduce institutional risk for buyers, accelerating procurement approval.
World Economic Forum analysis highlights that AI deployments succeed more often when vendors participate in governance design, including escalation protocols, override logic, and auditability frameworks.
Vendors that position themselves purely as technology suppliers face higher churn, even when their models outperform competitors in controlled evaluations.
Our perspective as a development service vendor
This vendor overview combines insights from cited sources with our own perspective as a software development service provider.
As a small boutique agency, we have learned how to operate effectively within the constraints and opportunities of SME-scale businesses.
Over the years, we have built and sustained a reliable network of clients by focusing on consistency, delivery, and long-term collaboration.
While we have not led a healthtech project from inception, we have contributed as an external augmentation partner on multiple global enterprise healthtech initiatives.
Through these engagements, we have supported core development efforts, aligned with established compliance and delivery standards, and worked within complex, large-scale systems.
Based on this experience, we view our work as aligned with the capabilities demonstrated by leading healthcare development service vendors in the market.
